BY MATTHEW GU
4. Prevention
Vaccines are the most effective and vital ways to prevent EVD. I will go into
vaccination efforts later on in chapter 6.
Dead bodies remain infectious therefore people handling human remains in practices
such as traditional burial rituals or more modern processes such as embalming are
at risk (CDC, 2014). Of the cases of Ebola infections in Guinea during the 2014
outbreak, 69% are believed to have been contracted via unprotected (or unsuitably
protected) contact with infected corpses during certain Guinean burial rituals (Chan,
2014) (WHO). Moreover, healthcare workers treating Ebola patients are at greatest risk of infection
(CDC, 2014). This risk rises significantly if they do not wear appropriate protective
clothing e.g., gowns, masks, eye protection, gloves. There have been cases of Ebola
transmission in some African hospitals which reused hypodermic needles and had a
lack of access to running water (CDC, 2018). These precautions are also essential
for handling items contaminated by infected body fluids. Ebola viruses can be
destroyed by heat (60 °C for 45 minutes or boiling for five minutes), and surfaces can
be disinfected using alcohol-based products or bleach (WHO, 2014).
Bushmeat, referring to wild animals hunted for food, plays a significant role in the
transmission of Ebola virus. Certain species, including fruit bats, non-human
primates, and duikers, are considered natural hosts or intermediate carriers of the
virus. Fruit bats, in particular, are thought to be the primary reservoir for Ebola.
These bats carry the virus without showing symptoms and can transmit it to other
animals through saliva, urine, or faeces (Leroy et al., 2005).

Figure 4: Image of a fruit bat, one of 197 species of bats that make up the
suborder Megachiroptera.
When bushmeat from infected animals is hunted, handled, or consumed without
proper precautions, humans can come into direct contact with the virus. For
example, skinning, cutting, or cooking bushmeat can expose individuals to infected
blood or bodily fluids, facilitating zoonotic transmission (Leroy et al., 2004). In some
outbreaks, this initial spill-over from wildlife to humans has been traced back to the
consumption of improperly cooked meat or the handling of dead animals found in the
forest.
5. Diagnosis and treatment
Ebola is diagnosed using specific laboratory tests that detect the virus in a person’s
blood or other bodily fluids. When someone shows symptoms like fever, vomiting,
and bleeding, doctors may suspect Ebola, especially if the person has been in
contact with an infected individual or has recently travelled to an area with an
outbreak. However, because these symptoms can be caused by other diseases like
malaria or typhoid fever, testing is crucial to confirm the diagnosis (CDC, 2021).
Possible non-specific laboratory indicators of EVD include a low platelet count; an
initially decreased white blood cell count followed by an increased white blood cell
count; elevated levels of the liver enzymes alanine aminotransferase (ALT)
and aspartate aminotransferase (AST); and abnormalities in blood clotting often
consistent with disseminated intravascular coagulation (DIC) (Kortepeter, 2011).
Moreover, observing cell cultures from a persons’ blood using electron microscopy
will allow doctors to identify the filamentous shape of EVD.
The most common tests used are:
- PCR Tests: These tests detect the virus’s genetic material in the blood. They
are highly accurate and can confirm an infection within hours. - Antigen Detection Tests: These tests check for antigens made by the virus,
providing faster results, though they may be less precise than PCR tests. - Serological Tests: These look for antibodies produced by the immune
system in response to Ebola. They are typically used to confirm past
infections rather than diagnosing active cases (WHO, 2023).
In outbreak situations, portable laboratory equipment allows for quick testing in the
field, helping doctors isolate infected individuals and prevent the virus’s spread. Early
and accurate diagnosis is essential for timely treatment and controlling the outbreak
(Feldmann & Geisbert, 2011).
Ebola is treated through a combination of supportive care and specific antiviral
therapies. While recent advancements in medicine have significantly improved
survival rates, treatment focuses on managing symptoms and maintaining the
patient’s vital functions.
The primary approach to Ebola treatment is supportive care, which includes:
– Hydration: Replacing lost fluids and electrolytes through oral rehydration
solutions or intravenous (IV) fluids to prevent dehydration and organ failure.
– Managing Symptoms: Treating symptoms like fever, vomiting, and diarrhoea
to reduce stress on the body.
– Blood Pressure Stabilisation: Maintaining blood pressure and oxygen levels
to support organ function.
– Treating Secondary Infections: Administering antibiotics or antifungals to
prevent or manage infections that can occur in weakened patients (CDC,
2023).
In recent years, 2 specific antiviral treatments have been developed and approved
for Ebola:
– Inmazeb (REGN-EB3): A combination of monoclonal antibodies that target
and neutralise the Ebola virus, reducing its ability to infect cells.
– Ebanga (mAb114): A single monoclonal antibody derived from a survivor of
Ebola
These treatments are most effective when given early in the course of the illness.
They help the immune system target and eliminate the virus, reducing the severity of
symptoms and improving the chances of recovery (FDA, 2020).
6. 2014 Outbreaks and Global effects
The 2014 Ebola outbreak was a global threat posed by the virus, emerging in Guinea
as the largest and deadliest outbreak since its discovery 40 years earlier. The
disease rapidly spread to the neighbouring countries of Liberia and Sierra Leone. It
was the largest Ebola outbreak ever documented, and the first recorded in the region
(CDC, 2014). Researchers traced the outbreak to a 1-year-old girl who had died in
December 2013 (Baize, 2014). The scale of the outbreak overwhelmed local
healthcare systems leading to international panic and just to put into perspective how
severe the 2014 outbreak was, I made the following bar chart to visualise the
number of deaths per annual period.
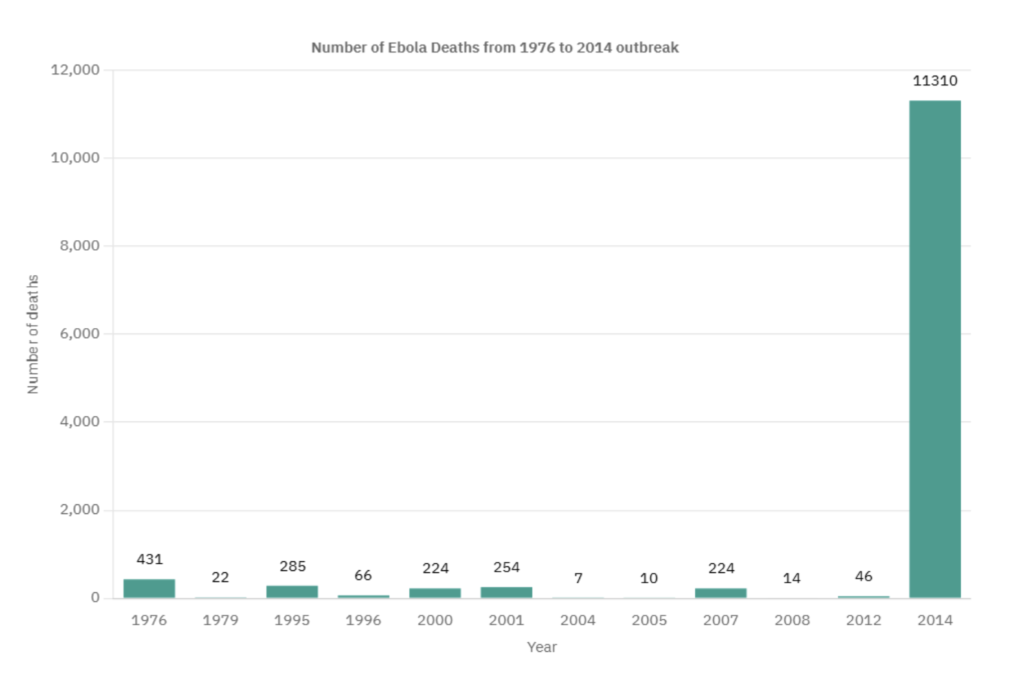
Figure 5: Graph showing the number of Ebola deaths per annual period from 1976 to
2014.
An Ebola vaccine called rVSV-ZEBOV was approved in the United States in
December 2019 and was shown to be fully effective ten days after administration
(Regules et al., 2015). It was first studied in Guinea between 2014 and 2016 (Henao-
Restrepo et al., 2017), and by 2019, over 100,000 people had been vaccinated
(WHO, 2019). During the Kivu Ebola epidemic from 2018 to 2020, the World Health
Organization reported vaccinating approximately 345,000 people (WHO, 2020).
The UK also played a critical role in vaccine development, led by Professor Adrian
Hill of the University of Oxford’s Jenner Institute. In September 2014, the Jenner
Institute began clinical trials of a candidate vaccine co-developed by NIH and GSK.
These trials were fast-tracked, supported by funding from the Wellcome Trust, the
Medical Research Council (MRC), and the Department for International
Development (DFID) (Wellcome Trust, 2014). Ruth Atkins, a 48-year-old NHS
worker, became the first volunteer to receive the vaccine in Oxford. She expressed
her hope that the trial would help alleviate the suffering caused by the outbreak in
West Africa. The vaccine used a benign protein from the virus to stimulate an
immune response, ensuring it could not cause infection. Early trials were designed to
evaluate its safety before larger-scale deployment in at-risk populations (University
of Oxford, 2014).
The urgency of the crisis led to an unprecedented global collaboration. In addition to
UK trials, related trials were conducted in the USA, The Gambia, and Mali to ensure
the vaccine’s safety across diverse populations (National Institute of Allergy and
Infectious Diseases, 2014). Manufacturing of thousands of doses began even before
trials concluded, in anticipation of a successful outcome.
This outbreak caused significant mortality, with a considerable case fatality rate. By
the end of the epidemic, 28,616 people had been infected and of these, 11,310 had
died (40% fatality rate) (Wappes, 2019). On 29 December 2015, 42 days after the
last person tested negative for a second time, Guinea was declared free of Ebola
transmission (CBC Reuters, 2015).
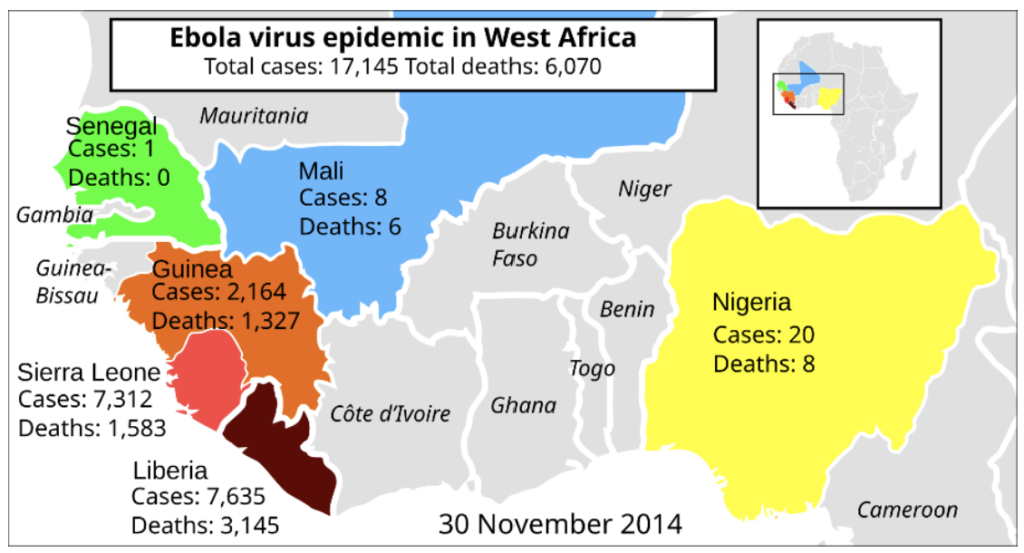
Figure 6: Map of West Africa showing cases and deaths of the 2014 EVD outbreak.
On 19 September, a man named Eric Duncan flew from his native Liberia to Texas;
five days later he began showing symptoms and visited a hospital but was sent
home. His condition worsened and he returned to the hospital on 28 September,
where he died on 8 October. Health officials confirmed a diagnosis of Ebola on 30
September – the first case in the United States (Botelho, 2014).
In early October, Teresa Romero, a 44-year-old Spanish nurse, contracted Ebola
after caring for a priest who had been repatriated from West Africa. This was the first
transmission of the virus to occur outside Africa (MSN). Romero tested negative for
the disease on 20 October, suggesting that she may have recovered from Ebola
infection.
On 12 October, the Centres for Disease Control and Prevention (CDC) confirmed
that a nurse in Texas, Nina Pham, who had treated Duncan tested positive for the
Ebola virus, the first known case of transmission in the United States (Fernandez,
2014). On 15 October, a second Texas health-care worker who had treated Duncan
was confirmed to have the virus. Both of these people recovered (CDC, 2014).