BY MATTHEW GU
5. Friday:
My final day began much like Thursday, with an early morning ward round at John Radcliffe Hospital. We saw C (14), a patient with benign fibrous dysplasia in her right leg, a condition where fibrous tissue develops in place of normal bone. Surgical excision to remove the growth was not required; the plan was to insert metal plates to stabilise the area and support the natural reduction of the dysplasia over time. The mother expressed her doubts and had to be reassured by the surgeon of the safety.
As with previous surgeries, the team convened again for the pre-operative WHO surgical checklist. (M)’s extensive surgery from the day before had taken six hours, yet the surgical team had immediately gone on to perform a smaller pin removal procedure afterwards. It was a powerful reminder of the endurance and dedication that defines surgical practice.
Following the morning round, I took some time to walk around John Radcliffe, reflecting on the experiences I’ve had and the journey that lies ahead of me. There’s a kind of magic in hospitals like this where science, compassion, and human stories all intersect. After this quiet moment of reflection, I made my way to the NOC for my final placement activity of the week.
There, I joined Senior Radiographer SH and Extended Scope Paediatric Physiotherapist LLS in screening newborns for DDH using ultrasound imaging. I was introduced to two key techniques:
- The Morin et al. method, used to evaluate the coverage of the femoral head within the socket.
- The Graf method, which involves measuring the alpha angle (an indicator of acetabular development). A normal alpha angle is approximately 60 degrees, and deviations from this may suggest shallow sockets or DDH. In some cases, a misreading can be corrected by adjusting pressure during scanning, but persistently low values may confirm a diagnosis.
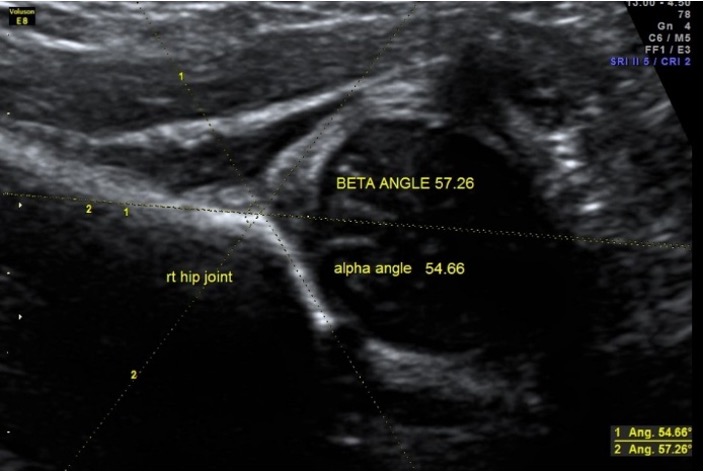
Figure 10: Ultrasound side view of the femoral head and acetabulum marked with angles.
Throughout the morning, we scanned seven babies, ranging from four weeks to two months old. Several were twins, and some were returning patients already undergoing treatment with Pavlik harnesses to encourage proper acetabular development. The process was smooth and meticulous as ultrasound gel was applied to aid transmission. A short flexion evaluation of the hips was then also given to assess movement.
This week has been an incredible journey into the world of orthopaedics. While many are drawn to fields like cardiothoracic surgery or neurosurgery, paediatric orthopaedics often sits quietly in the background. But after just one week immersed in it, I’ve come to truly appreciate its intricate nature and profound impact. After all, bones and muscles are the scaffolding of life.
What makes surgery, especially in children, so powerful is that it offers something beyond physical healing. It offers hope. A chance at walking again. At playing. At growing up with strength and confidence. No one can truly understand a paediatric patient’s story as deeply as they do themselves because each case is individual, personal, and deeply evocative. Every surgical journey is unique. Mine gave me a second chance. And now, after seeing so many others go through their own, I feel even more inspired and humbled.
Thank you for reading. I’ve chosen to tone down the scientific detail throughout this reflection to make it accessible to a wider audience, anyone who can connect to the power of empathy, compassion, and human resilience.
“10 more years from now and I hope to visit the NOC again however this time not as a patient, not as a student, but as a surgeon.” – Matthew 12/04/2025.
- Bibliography:
“CP and ageing”. Scope. Archived from the original on 6 May 2016.
Jenks KM, de Moor J, van Lieshout EC, Maathuis KG, Keus I, Gorter JW (2007). “The effect of cerebral palsy on arithmetic accuracy is mediated by working memory, intelligence, early numeracy, and instruction time.”
Nieuwenhuijsen C, Donkervoort M, Nieuwstraten W, Stam HJ, Roebroeck ME (November 2009). “Experienced problems of young adults with cerebral palsy: targets for rehabilitation care.”
“Orthopaedic Surgeons: Seven Things You Need to Know”. Penn Musculoskeletal and Rheumatology Blog. Philadelphia, PA: The Trustees of the University of Pennsylvania. 4 December 2019.
Oskoui M, Coutinho F, Dykeman J, Jetté N, Pringsheim T (June 2013).
Reference, Genetics Home (December 2014). “Williams syndrome”. Genetics Home Reference. Archived from the original on 20 January 2017.
Shaw, BA; Segal, LS; SECTION ON, ORTHOPAEDICS. (December 2016).